Patients Facing Death Are Opting for a Lifesaving Heart Device — But at What Risk?

Too old and too sick for a heart transplant, Arvid Herrman was given a choice: Have a mechanical pump implanted in his heart, potentially keeping him alive for several years, or do nothing and almost certainly die within a year.
The 68-year-old Wisconsin farmer chose the pump, called a HeartMate 3 — currently the only FDA-approved device of its kind in use. Instead of extending his life, though, the device led to his death, according to a lawsuit filed in December 2020 by his daughter Jamie Edwards.
The lawsuit alleged that Herrman died because a defect in the locking mechanism of the HeartMate 3 prevented the device from sealing, causing multiple strokes and leading to a severe brain injury and multiorgan failure. Herrman “could not have anticipated the danger this defect … created for him,” the lawsuit said.
Herrman’s death was reported to a Food and Drug Administration database where the public can learn about device-related deaths, serious injuries, and malfunctions. The event was also described in the peer-reviewed Journal of Heart and Lung Transplantation.
In September 2021, Ramon Flores Sr. had the same device implanted at Methodist Hospital of San Antonio. A lawsuit his family filed in August alleges that the locking mechanism defect led to air embolism strokes. Flores died eight days after surgery, at age 76.
“How many other people is this going to happen to?” said his daughter, Alanna Flores Blanco, 52. “We never, ever were explained that the device could malfunction and this could happen.”
After the deaths of Herrman and Flores, Thoratec Corp., the device’s manufacturer, evaluated the pumps involved. In both cases, Thoratec, a subsidiary of Abbott Laboratories, confirmed a bent locking arm. But “a direct correlation” between the HeartMate 3 and the deaths “could not conclusively be established,” the manufacturer reported to the FDA.
Abbott did not respond to questions about the deaths or the alleged defects. The manufacturer denied liability in both cases. It settled Herrman’s lawsuit this fall, and the Flores case is ongoing.
The men’s deaths are among more than 4,500 reports since August 2017 in which the HeartMate 3 may have caused or contributed to a patient’s death, according to a KFF Health News analysis of the FDA’s database of medical device incidents, known as the Manufacturer and User Facility Device Experience, or MAUDE. Hospitals, doctors, and others report device-related deaths, serious injuries, and malfunctions to manufacturers, who are required to investigate and report cases to the FDA.
In nearly 90% of those 4,500-plus reports, Thoratec said it found no problem with the device or how it was used, according to a KFF Health News review of the FDA database.
In cases where Abbott finds the HeartMate 3 did not cause or contribute to a death or serious injury, the company files “corrective reports,” said Justin Paquette, an Abbott public affairs director.
He added, “The complexity of the device – combined with patients battling late stage heart failure and associated comorbidities – creates very dynamic clinical care situations.”
Abbott said the HeartMate 3 is the safest iteration yet of any left ventricular assist device, or LVAD, a type of mechanical heart pump introduced in the 1960s and refined over the last six decades.
The HeartMate 3 was first approved by the FDA, for use in patients awaiting a heart transplant, in August 2017, and one year later it was approved as a long-term therapy. The device is often considered only for patients with end-stage heart failure, and even then it is a last resort.
HeartMate 3 has “dramatically improved the safety of LVADs by reducing rates of complications that had historically challenged heart pump technology, including clotting, stroke and bleeding,” Paquette said.
As recently as August, the FDA also expressed support for the device. “The FDA believes the benefits of HeartMate 3 continue to outweigh the risks for this vulnerable patient population with few available alternatives,” said Jeremy Kahn, an agency spokesperson.
Others aren’t so sure. Former FDA medical device official Madris Kinard sees the high number of death reports as a warning.
“To me this is a safety signal and it’s hard to know if the FDA is working on something to address it,” said Kinard, founder of Device Events, a company that makes FDA device data more user-friendly for hospitals, law firms, investors, and others. “You have to wonder why [death reports are] still happening, and at the same rate.”
Larry Kessler, a former director in the FDA’s medical device office, agrees the death reports for HeartMate 3 need more study. “The FDA may be missing some signals,” he said. Perhaps “there’s a little more here than meets the eye.”
Not all device problems are reported to MAUDE, and submitting a report is not necessarily an admission that a device caused a death or a serious injury. Device problem reports can be inaccurate or incomplete, or lack verification, and a single incident may be reported more than once — or not at all.
Those limitations ultimately can leave patients and their caregivers uninformed about risks associated with a device such as the HeartMate 3, said Sanket Dhruva, a cardiologist and expert in medical device safety and regulation at the University of California-San Francisco.
“They’re making perhaps the biggest decision of their lives: Do I proceed with an LVAD or not? And even if I proceed, what are the risks I’m facing?” he said. “And they are left with incomplete data and uncertainty about how to make that determination.”
Even doctors cannot use the FDA database as a tool to effectively counsel patients, Dhruva added.
“lf you don’t know what is a real safety signal and what’s not,” he said, “then how can that information help us to calibrate our benefits-and-risks discussion with patients?”
Tracking Incident Reports
The HeartMate 3 is not the only device whose safety profile is hard to ascertain in MAUDE, Dhruva said. The information in the FDA database is insufficient to give patients an adequate understanding of any medical device’s safety risks and reflects “the overall weakness of postmarket surveillance” after a device has been approved for sale, he said.
Under federal regulations, device manufacturers typically must report adverse events to the FDA within 30 days of learning about them, and that data is often used by researchers and regulators to identify potential safety concerns. Reports also can be submitted voluntarily by doctors, patients, or others. The FDA says that reports don’t need to be filed if the manufacturer determines that a device did not cause or contribute to an adverse event.
More from the series
-
Patients Expected Profemur Artificial Hips to Last. Then They Snapped in Half.
Dec 5, 2023
-
Thousands Got Exactech Knee or Hip Replacements. Then, Patients Say, the Parts Began to Fail.
Oct 10, 2023
-
This Dental Device Was Sold to Fix Patients’ Jaws. Lawsuits Claim It Wrecked Their Teeth.
Mar 1, 2023
But with millions of reports for thousands of devices, it can be difficult to detect and prevent problems that put patients at risk.
Hospitals and surgeons also might self-censor what they report to manufacturers due to concerns about being sued, said Kessler, now a professor at the University of Washington.
“Health care facilities, and risk managers in particular, they aren’t always forthcoming with detailed data about events,” he said.
Reports in MAUDE show that patients with a HeartMate 3 have experienced adverse events, such as bleeding, infection, and respiratory failure, that the manufacturer warned were possible in its instructions for use.
About 400 reports cited infusion or flow problems with the HeartMate 3. In thousands of other cases, the manufacturer said it did not observe any problems with the device, making it even more difficult for a doctor or a patient’s family to understand the safety history of the product.
Reports in MAUDE also describe fatal incidents due to complications not mentioned in the manufacturer’s instructions, such as the locking mechanism malfunction. In one report, a patient died of smoke inhalation after an external battery charger caught fire.
Each report in MAUDE has dozens of data points and summaries describing what happened. What’s lacking in the database: context and details that would be useful for patients and doctors, such as the total number of devices in use and the name of the hospital where the event occurred.
Flores Blanco had never heard of MAUDE before her father’s surgery. Even if she had, it’s unlikely she would have found a locking mechanism issue amid the morass of records, much less anticipated what might happen.
Missed Signals?
A routine FDA inspection of Abbott’s manufacturing plant in 2017 showed that Thoratec had fallen behind schedule reporting adverse events, according to agency records obtained by KFF Health News under a Freedom of Information Act request.
The company updated training and hired additional staff to handle complaints submitted by hospitals, doctors, patients, and others, according to an inspection report. It provided the FDA inspector with “quantitative evidence” that late reporting to the FDA had decreased.
By October 2020, during a follow-up inspection, Thoratec was using a database to enter and process complaints and submit device reports electronically, according to an inspection report.
FDA inspectors did not cite any deficiencies with how Thoratec handled complaints after the visit. Inspectors noted the company had received 8,115 complaints related to the HeartMate 3 during the 12 months prior to the inspection in October 2020, the records show.
It’s not clear what the complaints concerned. Abbott did not respond when asked how many of the complaints led to an adverse event report to the FDA.
In Kinard’s view, device-makers in general often take longer than 30 days to investigate the root cause of an incident and frequently conclude that an adverse event was due to user error.
“They are using this regularly to downplay the problems with the device,” she said.

In Herrman’s case, a Thoratec representative was in the operating room and witnessed the incident, according to a deposition in the lawsuit. The company submitted a report to the FDA about Herrman’s injury within 30 days of the June 2019 incident.
Herrman’s surgeon, John Stulak, was experienced at implanting the device, according to the lawsuit, and he was also a principal investigator on the clinical trial that brought the HeartMate 3 to market. Stulak did not respond to interview requests. But, in 2020, he and two Mayo Clinic colleagues described Herrman’s case in The Journal of Heart and Lung Transplantation, where they noted the locking mechanism malfunction. “The lack of a tight seal from this defect resulted in the multiple subsequent air embolism events and irrecoverable neurological damage,” they wrote.
The article describes how Stulak replaced the device with a new one, but it was too late to prevent the injuries to Herrman. Thoratec submitted at least three follow-up reports to the FDA about the incident and said its investigation could not determine whether the HeartMate 3 caused Herrman’s death.
Herrman’s death certificate cites complications of ischemic heart disease. Flores’ death certificate says he died of cardiac arrest and hypoxic ischemic encephalopathy, or brain damage.
The FDA has had its own problems keeping the MAUDE database up to date.
The agency is years behind schedule on anonymizing and releasing adverse event reports for all medical devices.
Kinard said the FDA has yet to publicly release “millions” of follow-up reports that manufacturers have filed after their initial adverse event report for a medical device.
The FDA acknowledged that the agency is not up to date on public reporting but could not say how many reports are pending — for the HeartMate 3 or any device.
“We are currently working on redaction for public posting in MAUDE, of all supplemental reports dated 2021-2023,” said Kahn, the FDA spokesperson. “It is difficult to determine how many of those – pending redaction of supplemental reports – pertain to the subject device.”
FDA press officer Lauren-Jei McCarthy noted that, besides adverse event reports, the agency also monitors published literature, patients, patient advocacy groups, professional societies, individual health care providers, and other sources to determine whether further action is warranted.
“We review and take seriously all reports of adverse events associated with medical devices,” McCarthy said. She said patients and providers who use the HeartMate 3 “remain a high priority” and that the agency cannot comment on investigations.
A Last-Resort Treatment
Before he got a HeartMate 3 implanted in January 2022, Sid Covington, of Austin, Texas, said he had researched the device during years of medication therapy and cardiac rehabilitation to treat his congestive heart failure.
“I looked at case studies. I looked at a number of the different heart studies,” Covington said. “I looked at their marketing brochures and all that stuff, just whatever I could find.”
Covington, 76, said he was familiar with MAUDE and Intermacs, a private registry that tracks LVAD patients, but didn’t consult them. When he had to decide whether to get the device, he was in the hospital with chest pain, shortness of breath, and fatigue from advanced heart failure. Covington said his only option was the HeartMate 3.
“When it comes down to the moment, you really don’t have much choice,” he said. “It’s any port in the storm at that point.”

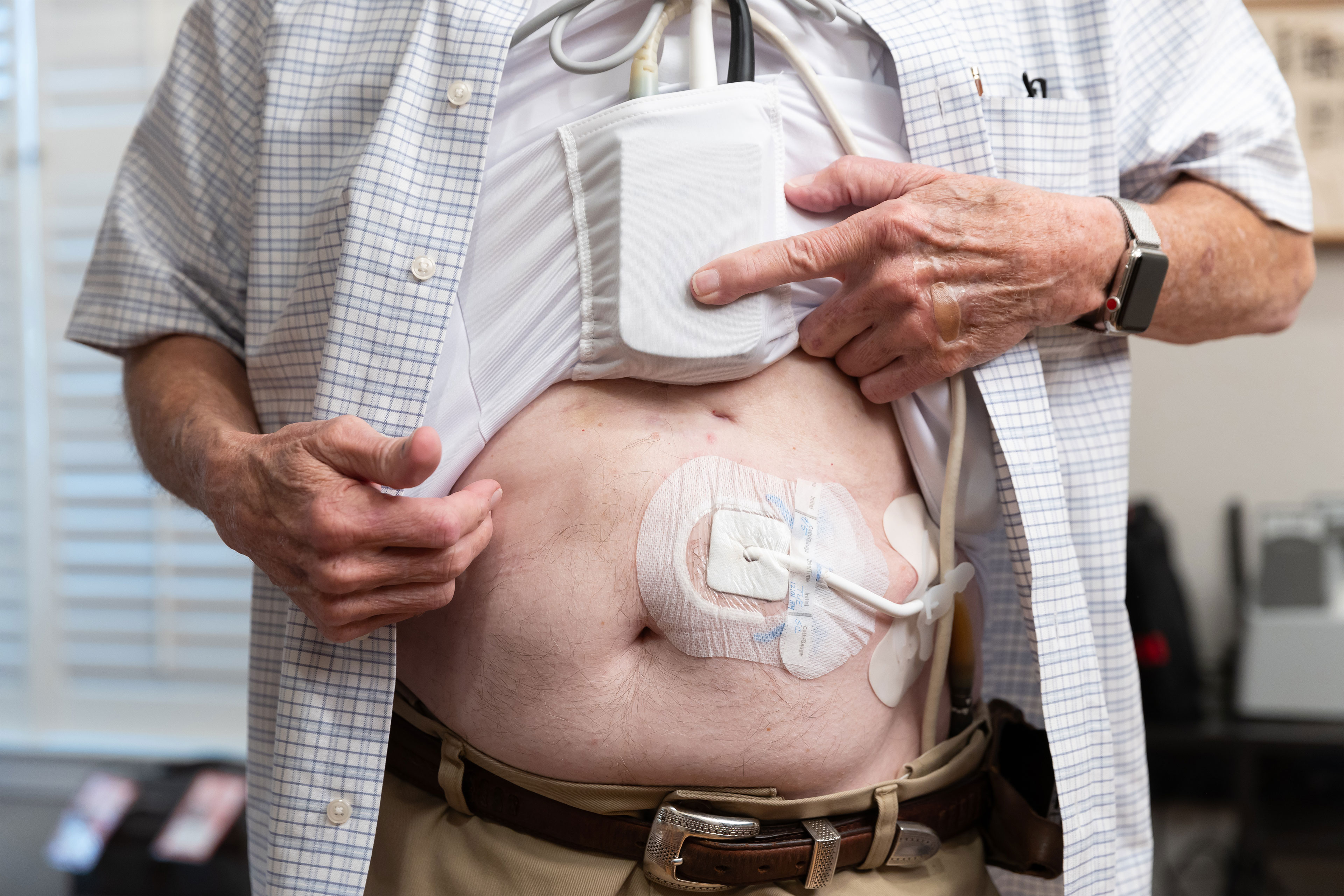
The HeartMate 3 requires constant attention and care from patients, who must keep the external parts of the device dry at all times and avoid jumping and contact sports. Patients must also ensure that it always has an external source of power, which is supplied through a cord attached to the pump that exits the body through a surgical opening.
Patients who get the device are often out of options to treat their end-stage heart failure, said Larry Allen, a cardiologist with the University of Colorado and member of a multidisciplinary medical team that cares for heart failure patients.
“We wouldn’t proceed with an LVAD unless we think the risk of death is really high and we’ve tried everything else,” he said.
That informs the regulatory view, too, Kessler said.
“When you’re talking about people who are seriously ill, then the FDA will accept a potentially higher risk,” he said, “but not an irresponsible one, and certainly not one that couldn’t be communicated to clinicians and the public.”
Allen, who helped develop a decision aid for patients considering an LVAD, said reliable data on safety and risks to patients is key.
“It’s about as high-risk, high-reward a choice as there can be,” Allen said. “It’s a really complicated decision to make and I think standard informed consent approaches are really inadequate for fully understanding that.”
Data Exists but Is Confidential
Long-term data for the HeartMate 3 — including performance metrics for the more than 180 U.S. hospitals certified to implant the device — are kept in Intermacs, managed by The Society of Thoracic Surgeons, which has promised to provide transparency but has yet to deliver.
The registry tracks mortality and injury rates for patients with an LVAD and logs the number of devices implanted each year.
But Intermacs is proprietary, and access at hospitals requires a principal investigator and at least one trained staff member, who can use the data to evaluate their facility’s performance against an aggregate from their peers across the nation.
Francis Pagani, a heart transplant and LVAD surgeon at University of Michigan Health, leads a medical society task force that oversees Intermacs. He said 12,000 to 14,000 HeartMate 3 implants have been recorded in Intermacs since 2017. The HeartMate 3 has “the best outcomes of any other LVAD, ever,” he said.
Over the years, federal regulators have made it easier for patients to access LVADs, reducing surgery volume requirements for implant centers and no longer requiring patients to be on a transplant waiting list to receive one of the pumps.
Though the HeartMate 3 is presently the only LVAD being implanted in the United States, it once had a competitor, Medtronic’s HeartWare, which the manufacturer removed from the market in June 2021, citing a high risk of stroke and pumps failing to restart if stopped.
While the FDA provides consumers with concise information about key clinical trials supporting the approval of new drugs, the agency provides no comparable data for medical devices. And though Medicare reimburses hospitals nearly $200,000 for most HeartMate 3 implants, federal administrators do not track patient outcomes or enforce performance standards for the heart pumps.
James Kirklin, a cardiac surgeon and researcher, was the principal investigator for Intermacs when the FDA, Centers for Medicare & Medicaid Services, and National Heart, Lung, and Blood Institute awarded a contract to the University of Alabama at Birmingham to establish the registry in 2005.
Federal agencies paid about $15 million over 10 years for Intermacs, Kirklin said, because they wanted to better understand the risk factors for death and other adverse events with so-called mechanical circulatory support devices, including LVADs, as well as the factors that indicated a higher likelihood of patients doing well on the pumps.
The FDA monitors annual reports of Intermacs data, including adverse events, and allows companies to use the registry’s data to analyze their devices’ performance and to fulfill reporting requirements after a device enters the market.
LVAD implant centers are required to report their data to Intermacs in order to be certified by the accrediting nonprofit The Joint Commission. And while CMS requires that centers implant at least 10 devices every three years to continue receiving Medicare reimbursement, there are no requirements for outcomes or other quality metrics. CMS does not track LVAD patient outcomes at individual facilities, said Sara Lonardo, CMS press secretary at the time.
Kirklin said he is working with The Society of Thoracic Surgeons to create a risk model that would allow the public to see quality scores for individual hospitals that implant LVADs, a need the group has recognized since at least 2018. But it will be a year before the tool is ready.
Kirklin and Pagani said the number of death reports for the HeartMate 3 in the FDA’s MAUDE database can be misleading without the outcome and longitudinal perspective that Intermacs provides.
“When you see a lot of deaths it means, ‘Let’s investigate.’ I couldn’t agree more,” Kirklin said. “But it’s rather limited. It’s not time-related and you don’t know the denominator. If you look up Intermacs, it’s all there.”
The families of Herrman and Flores filed lawsuits, in part, to find out what went wrong. Herrman’s family settled the lawsuit and agreed to confidentiality. Thoratec has filed a motion to dismiss the ongoing Flores case based on the FDA’s approval of the device.
Alanna Flores Blanco said she and her father were aware of the HeartMate 3’s positive outcomes, including published research that shows those who receive the device have a better than 50% chance of living five years or more.
“That’s why he took the chance to do it,” she said.
Flores Blanco said her father was a model patient, meeting regularly with cardiologists and other specialists, attending classes to learn how to live with the device, and receiving approval for surgery from the medical review board at Methodist Hospital in San Antonio.
The family felt informed and her father was prepared, she said.
“He did everything he was supposed to do,” she said. “What failed him ultimately was that device.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).

